Integration of human rabies surveillance and preventive measures in the State of Ceará, Northeast Brazil
Abstract
Aim: To analyze the One Health approach regarding rabies surveillance, control, and prevention in Brazil’s Ceará State, exemplified by a detailed description of rabies cases that occurred over 18 years.
Methods: We described in depth the history, case development, surveillance, and prevention measures of all cases of human rabies, 2004-2021. We analyzed patient charts and reviewed technical reports of the State Health Secretariat, in addition to analysis of personal notes from field missions.
Results: All six cases occurred in rural areas. The affected people came from resource-poor communities. The state rapid response team performed comprehensive actions and seminars in collaboration with the Municipal Health Secretariats and other stakeholder groups. Patients and their relatives were not aware about the risk of wildlife-mediated rabies. A high number of wild animals (marmosets) kept as pets were collected in the communities. Only one patient presented at a primary health care center before the onset of symptoms but did not receive any post-exposure prophylaxis due to logistic problems. Even after onset of symptoms, in all cases, the suspected diagnosis was not rabies at first. In four cases, transmission occurred by marmosets (Callithrix jacchus), one by a hematophagous bat (Desmodus rotundus), and another by a domestic dog, though the identified viral strain was sylvatic. All patients died.
Conclusion: Rabies in Ceará is a wildlife-mediated disease of the most vulnerable rural populations. There is a need for ongoing integrated surveillance and control measures, information and education campaigns, and professional training, especially focusing on wildlife-mediated rabies. An integrated One Health approach - as exemplified by the presented rabies control program in Ceará - is critical for human rabies elimination.
Keywords
INTRODUCTION
Rabies is a neglected tropical disease with considerable impact, mainly on resource-poor and disadvantaged populations. The World Health Organization’s most recent roadmap “Ending the neglect to attain the Sustainable Development Goals: a road map for neglected tropical diseases 2021-2030” targets elimination of rabies as a public health problem, to be evidenced by 92% of the countries having achieved zero human deaths from rabies by 2030[1].To achieve the elimination of rabies as a public health problem worldwide, it is necessary to adapt strategies at regional and national levels, to increase financial investment, and to apply measures according to specific local conditions[2-4].
As a result of regional efforts and the ongoing support by the Pan American Health Organization, systematic rabies control measures were strengthened in Latin America since the 1980s, and canine cases were reduced by 98%[4,5]. Human rabies still persists on the continent, and some areas register canine rabies. On the other hand, in some other areas there is an increasing importance of sylvatic animals for transmission, such as hematophagous bats[4,6,7].
Rabies control programs usually have focused on vaccination of dogs and cats as main transmitters, and often did not fully consider interdisciplinary approaches including humans, domestic animals, sylvatic animals, and the environment. While classically rabies control measures include vaccination and awareness campaigns, One Health approach integrates all major stakeholder groups and integrates more comprehensive activities. Thus, some authors have called for a One Health approach to further improve effectiveness of rabies control and prevention measures[8].
In Brazil, animal rabies surveillance and control measures are coordinated by the Ministry of Health and the Ministry of Agriculture and Livestock, in an integrated way, consisting of disease surveillance in dogs and cats, cattle, horses and wild species such as bats. There are still human rabies cases in the country; from 2010 to 2020, there was a total of 39 registered cases (all confirmed by laboratory diagnosis), with about half of them transmitted by bats, only around a quarter by dogs, 10% by cats, and another 10% by non-human primates[9]. Nowadays, hematophagous bats (Desmodus rotundus) and marmosets (Callithrix jacchus) are considered the main aggressor species for rabies virus transmission to humans in Brazil[10,11].
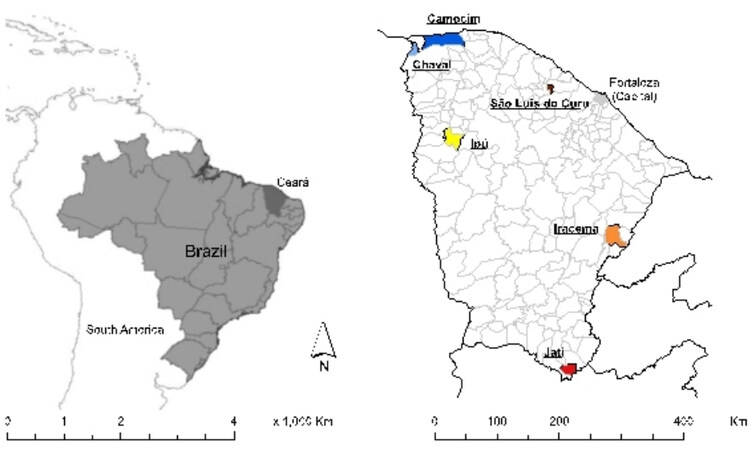
Ceará State in Northeast Brazil consists of 184 municipalities [Figure 1]. The population size is approximately 9 million, in an area of 149,000 km². The state is mainly characterized by savannah/caatinga vegetation, with exception of some Atlantic rain forest remains. The integrated program for rabies control was implemented in Ceará State in 2008. Since then, both the State Health Secretariat and the State Livestock Authority (ADAGRI) have put a strong emphasis on interdisciplinary and transdisciplinary aspects to improve rabies surveillance and control for humans, domestic animals, and wildlife. There is a multidisciplinary state rapid response team composed of about 10 professionals, including veterinarians, nurses, pharmacists, community health agents, endemic control agents, and health educators, who immediately visit the affected community and perform field investigations after the notification of a case. They remain in the field until the risk situation is controlled. The measures performed during these field missions include case investigation, contact tracing and post-exposure prophylaxis for exposed people, vaccination of people at risk, information and education campaigns, seminars for health professionals, vaccination of domestic and farm animals/livestock, laboratory analysis of suspected domestic and wild animals, viral strain identification, and collection of wild animals kept as pets in the communities.
Figure 1. Location of Ceará State in Northeast Brazil, highlighting the municipalities where the rabies cases occurred, 2004-2021.
As a way of implementing rabies surveillance and control in the state, several training activities were developed, such as courses, workshops, seminars, research studies, and institutional partnerships. The training activities of the integrated program for the control and surveillance of rabies in Brazil’s Ceará State are detailed in Table 1. The trainings were mainly carried out reactively, during the occurrence and investigation of human cases.
Training measures as elements of the integrated program for the control of rabies in Ceará State
| Rabies surveillance techniques | Theoretical and practical courses were delivered to all state veterinarians working in the public health sector. Seminars included collection and shipping of samples from dogs, cats, farm animals and sylvatic animals that died with neurological disorders, by cervical spinal cord collection technique. In addition, the State Livestock Authority held refresher courses on the identification of hematophagous bats and the collection and shipping of samples of farm animals |
| Technical professional training | Seminars for professionals of the technical rabies control teams throughout the state included identification of the main bat species of epidemiological importance, and aspects regarding the ecology, public health, and management measures for the control of diseases transmitted by these animals. Theoretical and practical courses were given on the implementation of the program for the prevention and control of rabies in bats, covering several Regional Health Coordinators for all veterinary medical professionals, Coordinators of the Primary Care and epidemiology, supervisors, and primary health care agents who work in the rabies surveillance program in the state of Ceará |
| Surveillance of wildlife-mediated rabies | Courses on surveillance of wildlife-mediated rabies were conducted in the state’s Regional Health Centers, for all professionals working in surveillance of wildlife |
| Inclusion of education sector and general population | In order to raise awareness of the epidemiological situation of rabies in the region and to increase the level of information on ways of preventing the disease, the state held several workshops to implement the project “Health and education in the control of wildlife-mediated rabies in the state of Ceará”, in partnership with the Health Secretariat and Regional Education Coordinators. Priority was given to regions where circulation of the rabies virus in the wild animal population is known. In addition, the State Livestock Authority carried out health education activities in rural communities on rabies in farm animals |
| Research in collaboration with academic institution | Collaboration of state authorities with the University of São Paulo included research on rabies in sylvatic animals. Academic trained professionals of the rabies control program on specific aspects of wildlife-mediated rabies, collection of biological material, and use of personal protective equipment |
| Training on rabies surveillance and clinical aspects | Refresher seminars were conducted for health professionals across the state (physicians and nurses) on clinical aspects and rabies surveillance |
| Training of physicians, nurses Primary health care workers Community health agents, and endemic control agents | Due to the high turnover of primary health care professionals responsible for the prescription of human anti-rabies protocol, meetings were held with the Regional Health Coordinators Seminars were conducted for physicians and nurses on standardized prophylactic treatment, according to the Ministry of Health’s guidelines Theoretical and practical courses for community health agents and endemic control agents focused on the prevention of rabies, such as animal vaccination, patient monitoring, post-exposure prophylaxis, and general aspects of endemics and their control |
| Collection of wild animals kept as pets | Collaboration with the Brazilian environmental authorities (IBAMA) in the collection of wild marmosets, capuchin monkeys, wild dogs, raccoons and other mammals, which are raised as pets by the population. Awareness campaigns were conducted, targeting the general population in high-risk areas. It is forbidden by law to keep wild animals as domestic animals |
In this paper, we describe the practical aspects of the above-mentioned integrated approach.
METHODS
We describe in detail the history, case development, and surveillance and prevention measures of all cases of human rabies that occurred in the state in the period 2004-2021.
We analyzed charts of the patients admitted to the state reference hospital for infectious diseases in the state capital Fortaleza. Five rabies patients of this study were admitted to this hospital. One patient was not transportable and was admitted to the regional hospital in Barbalha municipality. In this case, the expert team from the reference hospital supported the regional hospital team in clinical management.
In addition, we reviewed technical reports of the State Health Secretariat, and provided information from personal notes, as two of the authors (Duarte NFH & de Oliveira Moreno J) participated as members of the team in the investigations, as well as prevention and surveillance measures.
In three cases, rabies was confirmed by RT-PCR ante-mortem by the Ceará State reference laboratory, and in all cases, diagnosis was confirmed post-mortem by direct immunofluorescence performed at the Pasteur Institute in São Paulo. Viral typing of samples was performed by the Pasteur Institute for all cases.
RESULTS
Six cases of human rabies were recorded in the state, in six different municipalities scattered around the state’s hinterland [Figure 1]. All cases occurred in rural areas, and affected people who came from isolated resource-poor communities. Figure 2 depicts the house of case #1 and the primary health care center in the community, which is exemplary of the low socio-economic conditions and the poor health care system in the affected communities.
Figure 2. (A) House of rabies case #1 in the rural area of São Luis do Curú municipality. (B) Primary Health Care Center of the community.
Demographic and disease-related characteristics of the individuals are presented in Table 2. Five of the six patients were males. In four cases, transmission occurred by marmosets (Callithrix jacchus), one by a hematophagous bat (Desmodus rotundus), and another by a domestic dog, though the identified viral strain was sylvatic. All patients were bitten by the rabid animals, mostly on the hand. In the three patients, where diagnosis was confirmed by RT-PCR ante-mortem in cerebrospinal fluid, hair follicle, and saliva, the Recife/Milwaukee treatment protocol was applied. All six patients died.
Socio-demographic and epidemiological characteristics of rabies cases in Ceará State (2004-2021)
| Variable | n | % |
| Gender | ||
| Male | 5 | 83.3% |
| Female | 1 | 16.7% |
| Age (years) | ||
| 9 | 1 | 16.7% |
| 11 | 1 | 16.7% |
| 16 | 1 | 16.7% |
| 26 | 2 | 33.3% |
| 37 | 1 | 16.7% |
| Profession | ||
| Schoolchildren | 3 | 50.0% |
| Farmer | 3 | 50.0% |
| Aggressor species | ||
| Marmoset | 4 | 66.7% |
| Dog | 1 | 16.7% |
| Bat | 1 | 16.7% |
| Aggression type | ||
| Bite | 6 | 100% |
| Location of lesion | ||
| Hand/wrist | 4 | 66.7% |
| Face | 1 | 16.7% |
| Ankle | 1 | 16.7% |
| Healthcare seeking | ||
| Did not seek medical attention | 5 | 83.3% |
| Sought medical attention (but no post-exposure prophylaxis administered) | 1 | 16.7% |
| Viral variant | ||
| Marmoset (AgVsagui) | 4 | 66.7% |
| Wild canids (AgV2) | 1 | 16.7% |
| Haematophagous bat Desmodus rotundus (AgV3) | 1 | 16.7% |
Table 3 describes the detailed history and development of cases, and the surveillance measures performed by the state’s rapid response team which started investigation immediately after notification. In all cases, the technical team of the State Health Secretariat collaborated intensively with the Municipal Health Secretariats, Regional Health Coordination, State Livestock Authority, Education Secretariat, and other authorities and organizations, for preparation of an action and control plan, surveillance, and viral analyses. The rapid response team performed comprehensive actions to prevent any additional cases, and to make the population aware of the rabies risk. A large number of wild animals (marmosets) kept as pets were collected in the communities.
History, case development and intervention measures for the rabies cases that occurred in Ceará State (2004-2021)
| Case #1 (2005), São Luis do Curú municipality |
| History: In October 2005, a 26-year-old man from the rural area climbed a tree near his home to pick up a marmoset and was bitten on the finger of his left hand. The animal disappeared into the forest and was not seen again. The man had been feeding the marmoset for a few days. When the marmoset did not accept the food anymore, he had decided to capture it |
| Case development: About two months after the bite, the man began to feel tingling, pain, and numbness in his hands. He complained of chills, fever, and dizziness, but did not seek medical care at the municipal health center. The signs and symptoms worsened, and the man was referred to the local hospital, where the suspected diagnosis of dengue fever was made. From there, he was referred to the regional hospital and due to worsening of clinical and neurological signs, from there he was referred to the state reference hospital for infectious diseases in the state capital Fortaleza. The mother only mentioned the animal contact when she arrived at the referral hospital, and the physicians administered anti-rabies serum to the patient. The mother reported that no one in the family knew that marmosets would transmit rabies, thus the son did not seek medical care after the bite. The patient died ten days after admission to the hospital in Fortaleza |
| Intervention: The rapid response team visited the neighborhood and performed active detection of people exposed and livestock bitten by bats. The members of the man’s family were vaccinated. As a means of further prevention, all dogs,cats and livestock in the community received anti-rabies vaccination. An information and education campaign was immediately initiated in the community, consisting of lectures to increase knowledge on forms of rabies prevention by sylvatic animals, emphasizing the risk of keeping marmosets as pet animals |
| Case #2 (2008), Camocim municipality |
| History: On 8th December 2007, a 16-year-old girl from the rural area tried to capture a marmoset sitting in a cashew tree in front of her house. She was bitten in the right hand. Her mother immediately washed the wound with a phytotherapeutic tincture containing Operculina alata, locally known as “tincture of jalapa” or “aguardente alemã”. The animal escaped and did not appear again |
| Case development: Twenty-three days after the bite, the girl developed myalgia and paresthesia in her arm, and was only then taken to a primary health care center. The physician prescribed anti-inflammatory drugs. Her general condition worsened, and the girl was taken to the regional reference hospital in Sobral municipality, where anti-rabies serum was administered. On 5th February 2008, she developed fever, irritability, headache, and dyspnea. On 6th February, the patient was referred to the state reference hospital in the capital Fortaleza and died on the next day. Only with the patient's arrival at the reference hospital, the family informed that the brother had also been attacked by the marmoset on the same day |
| Intervention: When the state’s rapid response team arrived, they identified the girl’s brother who was bitten at the ankle, when he tried to help his sister. He received immediately post-exposure prophylaxis and survived without any sequelae. Another 19 individuals who had been attacked by mammals recently, though without seeking any medical care, were identified during house-to-house visits in the community. Subsequently, training on anti-rabies prophylaxis was carried out for health professionals in the municipality. A comprehensive awareness campaign was rolled out, consisting of lectures on rabies in schools and in the community. The lectures focused on important aspects of rabies, such as animal reservoirs, type of transmission and prevention. In addition, interviews were conducted in local radio stations to increase awareness of the population on the risk of rabies, and on the importance of seeking medical assistance. Dogs and cats in eight close-by rural communities were vaccinated, and stray dogs were captured. A door-to-door survey on sylvatic animals raised as pets identified 51 marmosets. These were collected and handed over to the environmental authorities (IBAMA). Consequently, additional awareness campaigns were carried out on the risk of keeping sylvatic animals in captivity. The health secretariat of the municipality formed partnerships with the educational secretariat and civil society associations, and educational material was elaborated for distribution within the population |
| Case #3 (2010), Chaval municipality |
| History: On 21st May 2010, a 26-year-old man from the rural area, who used to take his dog for hunting in the savannah, applied a bandage to a wound on the back of his animal, possibly a result from a fight with a fox or a wild dog. At this occasion, he was bitten by his dog on the hand. To stop the bleeding, he washed the wound with ice water and salt. He went to the primary health care center, where asepsis and wound dressing were performed. He was requested by the health professional to return to the health clinic after the weekend, because at the moment there was no physician present to prescribe post-exposure prophylaxis. The patient returned on the 22nd and 23rd May (Saturday and Sunday) to change the dressing, and again he was informed about the importance of returning the next day for rabies prophylaxis, and to observe the animal for 10 days. Meanwhile, the dog attacked a domestic pig that was sacrificed and incinerated and three other dogs that received the vaccine. According to the aggressor animal's vaccination card, the dog had been vaccinated four years ago. It died on 30th May 2010, 9 days after biting his owner. The man claimed that the application of post-exposure prophylaxis for him was unnecessary, as he was not feeling anything, despite numbness in his hand |
| Case development: The man complained of myalgia and paresthesia at the site of the bite. However, he resisted family advice to seek medical attention. After two weeks, he developed fever. On 27th August, he complained of pain and numbness in his arm, sore throat, and difficulty sleeping. Four days later, he went to a primary health care center, presenting fever and sore throat, and received prescription of ibuprofen and amoxycillin. During medical consultation, he was not asked about any animal bites or contacts. On 1st September, the patient’s condition worsened, and he presented at the local hospital, with fever (39.5 °C), dark colored excessive salivation, dysphagia, aerophobia, psychomotor agitation, dysarthria, and dyspnea. After being informed about the dog bite without subsequent post-exposure prophylaxis, the physician referred the patient to the state reference hospital in Fortaleza. The patient died 18 days after the beginning of treatment according to the Recife Protocol |
| Intervention: The state’s rapid response team identified 10 individuals by active case finding in the community who had had contact with the diseased animal or the patient's saliva. As most of the animals in the community had not been vaccinated in years and due to the presence of wild canids in the localities, all dogs and cats in the municipality were vaccinated, with street animals being captured, vaccinated and placed in appropriate locations under the supervision of the veterinarian. Courses were held for health professionals on rabies prophylaxis. A meeting was held with all municipal councilors to pass on information about the case and request support in educational actions on rabies prevention and the importance of vaccination of dogs and cats; and to collect wild animals in captivity to be handed over to the environmental authorities |
| Case #4 (2010), Ipú municipality |
| History: In October 2010, the population of the municipality of Ipú burnt the fields to prepare the soil for planting, and many animals escaped from the fire to the urban area of the city. When leaving his house to work, a schoolteacher came across a marmoset (C. jacchus) sitting in a tree in front of his house. Two children who passed by, stopped and stood looking at the animal, and one of them (11-year-old boy) approached the tree. The animal jumped on his shoulder and hit him in the face, then jumped on the teacher's back and scratched him. According to the child's mother, she did not seek medical attention for the child because she was unaware of the risk, and the child had not presented any symptoms. Only after the appearance of signs and symptoms, the child was taken to the doctor |
| Case development: On 10th November, the boy had headache, fever, tiredness, drowsiness, fatigue, did not play with his brothers, and did not eat. On 16th November, the mother sought care at the local hospital. The physician diagnosed a severe migraine and released the patient. On the following day, the boy returned to the hospital with persistence of symptoms, and seizures. He was hospitalized for three days. On 20th November, the condition worsened, and the patient was transferred to the reference hospital in the region, in Sobral municipality, where the clinical diagnosis of rabies was made. There he remained until 22nd November, when he was transferred to the state reference hospital in the capital Fortaleza, where immediately the Recife Protocol was initiated. The boy died on 27th November |
| Intervention: Active case finding was done to identify individuals possibly exposed the rabies virus. These were identified with the help of the teacher and included 14 children who had been bitten by marmosets and a teenager attacked by a dog. All of them had not received any post-exposure prophylaxis and were referred to the primary health care center; none of them developed rabies. The teacher had not received post-exposure prophylaxis until the day the boy started having symptoms. In addition, the rapid response team identified families that kept wild animals in captivity; nine marmosets were collected and handed over to environmental authorities. An awareness campaign was started focusing on the risk of keeping sylvatic animals as pets and rabies transmission. Public and private schools were visited and videos presented and lectures held. Community health agents were trained. An evaluation showed that the knowledge of community health agents was poor in relation to rabies transmission and prevention. The community was shocked, and fear spread; parents did not let their children go to school, as the mode of transmission was not known in the community. People were afraid that their children would acquire rabies if they drank from the same water fountain, sat on the same chair, or by entering the classroom of the boy who died. In addition to interviews at local radio stations in Ipú and Sobral, lectures were held to the community on rabies transmission and prevention, and to create awareness |
| Case #5 (2012), Jati municipality |
| History: On 2nd February 2012, a group of children spotted a marmoset in a tree and knocked it down using a swing. A 9-year-old boy took the animal. When he tried to put it in his cap, he was bitten on the finger. Then he put the marmoset in a cage and hung it on the tree behind the house. On the following day, the boy approached the cage and when he stroked the animal's head, he was bitten on the thumb. The boy's grandmother washed the wound with water, soap and vinegar to stop the bleeding and told the grandson to get rid of the animal. The animal was released on a tree next to the house, and was found dead on the next day. The grandmother said that she did not take the boy to the primary health care center, as she was unaware of the risk caused by such a small wound |
| Case development: On 22nd February, the boy presented with fever and pain in the arm but was taken to the local hospital only on the following day. The pediatrician prescribed antipyretic and analgesic drugs, and ice compresses. He did not ask about any history of animal contact. In the subsequent three days, the boy remained with moderate fever, and lack of appetite. On 26th February, he presented episodes of frequent vomiting. The day after, he was taken again to the local hospital. Another day later, his general condition worsened. Until now, diagnosis the diagnosis was dengue fever. On 29th February, the physicians suspected meningitis and transferred him to the reference hospital in the region in Barbalha municipality. There, rabies was suspected for the first time, and family members were asked about animal contacts, which was confirmed to be happened about 27 days ago. The Recife Protocol was implemented immediately, but the boy died on 12th March |
| Intervention: The state rapid response team immediately conducted active case finding of individuals who had contact with saliva of the boy, or with the animal. The grandmother had contact with both, and on 4th March developed fever, nausea, vomiting, fatigue, and headache, but the diagnosis of rabies could be excluded. She was referred to the hospital in Jati and remained hospitalized, receiving post-exposure prophylaxis only administered on 7th March. The nursing technician and uncles had contact with the child's secretion, and seven children who were with him at the time of the aggression had contact with the marmoset. All exposed individuals underwent medical evaluation and received post-exposure prophylaxis. Educational video presentations and lectures were performed for schoolchildren. The primary health care teams assisted lectures on the epidemiological aspects of rabies, and post-exposure prophylaxis. During these lectures, the health professionals and also the population informed the rapid response team that several people, both in the rural and urban areas, would capture and keep wild animals as pets, mainly marmosets and capuchin monkeys. House-to-house visits in the community were carried out, to alert the population of the risk of keeping wild animals. A total of nine animals were collected (eight marmosets and a capuchin monkey) and delivered to the environmental authorities. The animals were microchipped and an oral swab was collected for antibody analysis, with negative result in all cases |
| Case #6 (2016), Iracema municipality |
| History: On 5th October, a 37-year-old farmer, living in the rural area was claiming of leg numbness and difficulty urinating. He reported being attacked by a hematophagous bat on 2nd September while sleeping. He woke up because he felt uncomfortable due to a burning ankle. When he turned on the bedroom light, he saw blood on the spot and on the bed sheet, and a bat struggling between the walls and wardrobe. He killed the bat, threw it into the waste bin and went back to sleep. The next day, his wife insisted seeking medical assistance, but he did not go to any health center |
| Case development: Since 5th October, the patient complained of weakness and pain in legs, headache, and vomiting. Only on 19th October, he sought medical care at the local hospital with complaints of feeling of full urine bladder, pain in the limbs, and lower back pain. The next day, he was referred to the reference hospital in Fortaleza, and was admitted with paresis in the left leg (site of the aggression - foot), which evolved to the other leg, and decreased muscle strength. The Recife treatment protocol was initiated on that day. He died on 11th November |
| Intervention: The rapid response team held meetings with technicians from the Municipal Health Secretariat, Regional, State Health Secretariat, and State Agricultural Defense Agency to develop an action plan, including: active case finding to identify suspected cases in humans and animals in the community and neighboring locations (within a radius of 18 to 20 km); provide guidance to the local population on preventive measures and management, in case of occurrence of aggressions by bats, dogs, cats, or monkeys; guidance to health professionals on how to collect the different bat species found at unusual places and periods, and to send them to the laboratory investigation; identification of bat shelters, and collection of hematophagous bats; intensification of canine and livestock farms rabies vaccination in all municipalities in the region; educating the population about human rabies through the municipality's radio; training on human rabies to municipality workers with a practical class to identify species and bats; survey and mapping of locations of bats; and identifying people who raised wild animals in captivity |
The case descriptions show that people in the communities were not aware of the risk of rabies being transmitted by wild animals, and sometimes even approached the diseased animals actively (cases #1, #2, #4, and #5). One patient was attacked by a hematophagous bat while sleeping (case #6). He was living in a simple house, with easy access for bats to the sleeping room [Figure 3]. Domestic animals were abundant around the house of this case [Figure 4]. This is remarkable, as usually, these bats prefer blood-feeding on animals and only feed on humans in the absence of adequate animals.
Figure 3. (A) House of rabies case #6 in the rural area of Iracema municipality. (B) View from inside the house evidencing easy access of hematophagous bats to the sleeping room.
Figure 4. Domestic animals around the house of case #6 who was attacked by a hematophagous bat (Desmodus rotundus).
Only one patient presented at a primary health care center before the onset of symptoms (case #3). He presented to the primary health care center for wound care, after being bitten by his hunting dog, but did not receive any post-exposure prophylaxis due to logistic problems; no physician was present at the weekend and he did not return to the health center thereafter. Even after onset of symptoms, in all cases, the suspected diagnosis was not rabies at first.
DISCUSSION
Our detailed description of the investigation of all human rabies that occurred during a period of 18 years in Ceará State demonstrates the need for ongoing integrated surveillance and control measures. All cases occurred in resource-poor communities with limited access to the educational and health systems, in the rural hinterland. Rabies in the state can be characterized as a rural wildlife-mediated disease of the mostly underprivileged populations, being one of the most neglected diseases in the region. The affected communities were not aware about the risk of wildlife-mediated rabies, there was limited access to the health system hampering timely administration of post-exposure prophylaxis, and the primary health care system did not adequately consider rabies as a differential diagnosis. The multidisciplinary state rapid response teams realized integrated measures including all stakeholder groups to prevent further cases.
In all cases, wild rabies virus strains were isolated. In fact, canine rabies has virtually been eliminated from Brazil[12]. Rabies used to be common in the state in domestic animals and in urban areas some decades ago, but due to intensive anti-rabies campaigns, transmission by dogs has been eliminated. In 2003, seven cases of human rabies were still registered, all of them transmitted by dogs. The last rabies case transmitted by a dog in the state occurred in 2010[13]. Transmission by wild animals, mainly by marmosets and hematophagous bats, increased since then, indicating the importance of integrated and continuous measures, especially regarding information and education campaigns.
Before implementation of the integrated measures, the state health department carried out rabies control together with the municipal health departments when there were cases of animal or human rabies notified. Rabies surveillance in wild animals consisted of collecting biological samples of dead animals found on state highways, such as wild canids and raccoons, for laboratory diagnosis. Since 2008, with the occurrence of more and more human cases transmitted by wild animals, especially marmosets, the focus was widened to non-human primates (especially marmosets and capuchin monkeys) kept as pets, in collaboration with environmental authorities (IBAMA). Activities included collection of animals and information and education measures. Subsequently, visits were made to the homes for awareness-raising about environmental legislation, disease risk, and animal welfare. Since then, the rabies control program of the state has been working continuously on awareness raising about the risk of raising wild animals as pets, performed seminars and courses on sylvatic rabies and surveillance methods for health professionals. Consequently, there was a reduction of human cases in recent years.
Surveillance of domestic and wild animals (including bats, marmosets, foxes, and other animals) is important to reduce the transmission risk[10]. Clearly, successful control and elimination of infectious diseases depend on effective disease surveillance, especially in the case of zoonoses, including rabies[14]. However, surveillance often is not given priority, due to other issues that seem to be more urgent in resource-poor settings[15]. Interdisciplinary surveillance would include surveillance of rabies virus in bats, in collaboration of health and agricultural authorities[10]. We have discussed recently the importance of passive surveillance of rabies virus in bats and marmosets being fundamental for rabies control in both humans and domestic animals in Brazil’s Ceará State[10].
Our study points out several bottlenecks in the implementation of the rabies control program, mainly regarding access to the health system, awareness of health professionals, and knowledge of the population on rabies transmission. Rabies symptoms and signs are often non-specific, and the disease is rare, which may explain the delayed diagnosis of the reported cases. Rabies should always be suspected in patients with neurological disorders, and professionals should ask about any animal contacts. Intensified and continuous professional education (health professionals, veterinarians, and primary health care agents) and information and education campaigns (communities at risk and schoolteachers) are important.
One focus of training for health professionals should be the correct application of post-exposure prophylaxis. For surveillance, the Brazilian nationwide health information system for notifiable diseases (called SINAN) registers patients seeking post-exposure prophylaxis. A nationwide study has shown that less than half of these received complete post-exposure prophylaxis according to Brazil’s Ministry of Health guidelines, and consequently better management of animal bites has been suggested[12]. Another nationwide study based on passive surveillance data has shown that in Brazil, only half of patients received the correct post-exposure prophylaxis[16]. A recent study from Ceará State identified 231,694 incidents involving animals. Of this total, 222,036 (95.8%) received no or incomplete post-exposure prophylaxis, as compared to the Ministry of Health’s prophylactic anti-rabies treatment guidelines[17]. Similarly, post-exposure prophylaxis in Haiti was very low, where only 31% of rabies exposed individuals had initiated post-exposure prophylaxis[15]. To achieve zero human deaths from rabies, universal access and availability of adequate post-exposure prophylaxis for all potential exposures will be needed.
The keeping of wild animals is prohibited by law in Brazil, but in collaboration with environmental authorities, the rapid response team identified and collected a high number of marmosets being kept as domestic animals in the communities. Thus, a major focus in education campaigns should be given to the sylvatic animals that transmit rabies to humans. Elimination of rabies in sylvatic animals is feasible in some settings. Oral rabies vaccine-containing baits are deposited in natural habitats. For example, wildlife-mediated rabies has virtually been eliminated from western Europe, as a result of oral rabies vaccination campaigns for foxes and raccoon dogs[18], and an additional control approach may consist of placing vaccine baits close to communities in rural areas, but laboratory and field research would be required to determine if such an approach would be effective and feasible in Ceará.
Control of neglected tropical diseases, and specifically rabies control within the One Health approach would include human health, social sciences, environmental, animal health, and wildlife sectors, embedded into a strong routine surveillance and reporting system[8,19]. Integrated measures depend on the specific settings, and may consist of pre- and post-exposure prophylaxis, adequate diagnosis, capacity building, reducing wildlife and domestic animal interactions, vaccination of domestic animals, and active and passive surveillance. All major stakeholder groups should be included, and the communities may be actively involved in surveillance actions. The focus on specific areas, and most vulnerable populations ideally would also include other neglected tropical diseases endemic in Brazil[20].
This multidisciplinary approach, as exemplified by the state rabies control program in Ceará, has been an important and successful step to improve surveillance and control actions. In Mexico, dog-mediated rabies has been eliminated, by implementing mass dog vaccination campaigns, effective surveillance, awareness-raising campaigns, and easy access to post-exposure prophylaxis[21]. Other countries, mainly in Asia where traditionally most human rabies have occurred, also successfully implemented the One Health approach, and reduced canine rabies and human cases significantly, such as in India where stray dogs pose major problem for rabies control[22], and in Nepal where its government adopted a nationwide One Health strategy for all relevant sectors, including zoonoses[8]. In China, the One Health approach has been recommended to integrate different disciplines and the different levels of rabies control - control of human rabies including strengthening of public awareness in high-risk rural populations and control of rabies in wild animals, livestock, and stray dogs, including surveillance[23]. Similarly, in Australia, which is free of canine rabies, One Health activities have been proposed to effectively prevent the reemergence of the disease[24]. In Sri Lanka, the One Health approach has been advocated, but there are still some obstacles for integrated measures, such as missing standardization of the control program, and insufficient harmonization of different areas involved[25]. While on the grassroots level, this is usually very effective, on the high rank political level, silo thinking may prevail, and interdisciplinary approaches are sometimes difficult to establish[26].Clearly, implementation measures should be tailored to the given epidemiologic, biological, cultural, and socio-economic context.
We conclude that there is an ongoing need for integrated surveillance and control measures in the state, for information and education campaigns, and professional training, especially focusing on wildlife-mediated rabies. An integrated One Health approach - as exemplified by the presented rabies control program in Ceará - is critical for human rabies elimination.
DECLARATIONS
AcknowledgmentsHeukelbach J is research fellow from Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq/Brazil).
Authors’ contributionsOriginal draft preparation: Heukelbach J, Duarte BH
Performed data acquisition: Holanda Duarte NF, Moreno JO, Duarte BH, Araújo Melo IML
Made substantial contributions to conception and design of the study and performed data analysis and interpretation, review and editing of the manuscript: Holanda Duarte NF, Alencar CH, Pires Neto RJ, Moreno JO, Araújo Melo IML, Duarte BH, Heukelbach J
All authors have read and agreed to the published version of the manuscript.
Availability of data and materialsNot applicable.
Financial support and sponsorshipNone.
Conflicts of interestAll authors declared that there are no conflicts of interest.
Ethical approval and consent to participateThe study was approved by the Ethical Review Boards of the Federal University of Ceará, of the State Health Secretariat, and of the state reference hospital for infectious diseases (Hospital São José). As the study consisted of analysis of secondary data and of description of personal experience of the authors, no informed consent was sought.
Consent for publicationAll images were taken by the authors, and the authors pertain the copyright.
Copyright© The Author(s) 2021.
REFERENCES
1. Vieri MK, Logora MY, Rafiq K, Colebunders R. The World Health Organization road map for neglected tropical diseases 2021-2030: implications for onchocerciasis elimination programs. Infect Dis Poverty 2021;10:70.
2. Wallace RM, Undurraga EA, Blanton JD, Cleaton J, Franka R. Elimination of dog-mediated human rabies deaths by 2030: needs assessment and alternatives for progress based on dog vaccination. Front Vet Sci 2017;4:9.
3. Vigilato MAN, Molina-Flores B, Del Rio Vilas VJ, Pompei JC, Cosivi O. Canine rabies elimination: governance principles. Rev Sci Tech 2018;37:703-9.
4. Freire de Carvalho M, Vigilato MAN, Pompei JA, et al. Rabies in the Americas: 1998-2014. PLoS Negl Trop Dis 2018;12:e0006271.
5. Vigilato MA, Cosivi O, Knöbl T, Clavijo A, Silva HM. Rabies update for Latin America and the Caribbean. Emerg Infect Dis 2013;19:678-9.
6. Benavides JA, Valderrama W, Recuenco S, et al. Defining new pathways to manage the ongoing emergence of bat rabies in Latin America. Viruses 2020;12:1002.
7. Galhardo JA, De Azevedo CS, Remonti BR, et al. Canine rabies in the Brazil-Bolivia border region from 2006 to 2014. Ann Glob Health 2019;85:25.
8. Acharya KP, Acharya N, Phuyal S, Upadhyaya M, Lasee S. One-health approach: a best possible way to control rabies. One Health 2020;10:100161.
9. Health BMO. Anger: what is it, causes, symptoms, treatment, diagnosis and prevention. Available from: https://antigo.saude.gov.br/saude-de-a-z/raiva [Last accessed on 21 Jun 2021].
10. Duarte NFH, Alencar CH, Cavalcante KKS, et al. Increased detection of rabies virus in bats in Ceará State (Northeast Brazil) after implementation of a passive surveillance programme. Zoonoses Public Health 2020;67:186-92.
11. Favoretto SR, de Mattos CC, de Mattos CA, Campos AC, Sacramento DR, Durigon EL. The emergence of wildlife species as a source of human rabies infection in Brazil. Epidemiol Infect 2013;141:1552-61.
12. Benavides JA, Megid J, Campos A, Rocha S, Vigilato MAN, Hampson K. An evaluation of Brazil's surveillance and prophylaxis of canine rabies between 2008 and 2017. PLoS Negl Trop Dis 2019;13:e0007564.
13. Duarte NFH, Pires Neto RDJ, Viana VF, et al. Epidemiology of human rabies in the state of Ceará, Brazil, 1970 to 2019. Epidemiol Serv Saude 2021;30:e2020354.
14. Townsend SE, Lembo T, Cleaveland S, et al. Surveillance guidelines for disease elimination: a case study of canine rabies. Comp Immunol Microbiol Infect Dis 2013;36:249-61.
15. Wallace RM, Reses H, Franka R, et al. Establishment of a canine rabies burden in Haiti through the implementation of a novel surveillance program. PLoS Negl Trop Dis 2015;9:e0004245.
16. Benavides JA, Megid J, Campos A, Hampson K. Using surveillance of animal bite patients to decipher potential risks of rabies exposure from domestic animals and wildlife in Brazil. Front Public Health 2020;8:318.
17. Cavalcante KKDS, Alencar CH. Human rabies: evaluation of post-exposure prophylaxis prevalence in Ceará, Brazil, 2007-2015. Epidemiol Serv Saude 2018;27:e2017547.
18. Müller FT, Freuling CM. Rabies control in Europe: an overview of past, current and future strategies. Rev Sci Tech 2018;37:409-19.
19. Heukelbach J. One Health & Implementation Research: improving health for all. One Health Implement Res 2021;1:1-3.
20. Martins-Melo FR, Carneiro M, Ramos AN Jr, Heukelbach J, Ribeiro ALP, Werneck GL. The burden of neglected tropical diseases in Brazil, 1990-2016: a subnational analysis from the Global Burden of Disease Study 2016. PLoS Negl Trop Dis 2018;12:e0006559.
21. World Health Organization. Mexico is free from human rabies transmitted by dogs. https://www.who.int/news/item/21-12-2019-mexico-is-free-from-human-rabies-transmitted-by-dogs [Last accessed on 21 Jun 2021].
22. Fitzpatrick MC, Shah HA, Pandey A, et al. One Health approach to cost-effective rabies control in India. Proc Natl Acad Sci U S A 2016;113:14574-81.
23. Tan J, Wang R, Ji S, Su S, Zhou J. One Health strategies for rabies control in rural areas of China. Lancet Infect Dis 2017;17:365-7.
24. Degeling C, Brookes V, Lea T, Ward M. Rabies response, One Health and more-than-human considerations in Indigenous communities in northern Australia. Soc Sci Med 2018;212:60-7.
25. Nihal PDB, Dangolla A, Hettiarachchi R, Abeynayake P, Stephen C. Surveillance opportunities and the need for intersectoral collaboration on rabies in Sri Lanka. J Vet Med 2019;2019:7808517.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Holanda Duarte NF, Alencar CH, Pires Neto RJ, Moreno JO, Araújo Melo IML, Duarte BH, Heukelbach J. Integration of human rabies surveillance and preventive measures in the State of Ceará, Northeast Brazil. One Health Implement Res 2021;1:17-30. http://dx.doi.org/10.20517/ohir.2021.02
AMA Style
Holanda Duarte NF, Alencar CH, Pires Neto RJ, Moreno JO, Araújo Melo IML, Duarte BH, Heukelbach J. Integration of human rabies surveillance and preventive measures in the State of Ceará, Northeast Brazil. One Health & Implementation Research. 2021; 1(1): 17-30. http://dx.doi.org/10.20517/ohir.2021.02
Chicago/Turabian Style
Holanda Duarte, Naylê Francelino, Carlos Henrique Alencar, Roberto da Justa Pires Neto, Jarier de Oliveira Moreno, Iva Maria Lima Araújo Melo, Bruna Holanda Duarte, Jorg Heukelbach. 2021. "Integration of human rabies surveillance and preventive measures in the State of Ceará, Northeast Brazil" One Health & Implementation Research. 1, no.1: 17-30. http://dx.doi.org/10.20517/ohir.2021.02
ACS Style
Holanda Duarte, NF.; Alencar CH.; Pires Neto RJ.; Moreno JO.; Araújo Melo IML.; Duarte BH.; Heukelbach J. Integration of human rabies surveillance and preventive measures in the State of Ceará, Northeast Brazil. One. Health Implement. Res. 2021, 1, 17-30. http://dx.doi.org/10.20517/ohir.2021.02
About This Article
Copyright
Data & Comments
Data

 Cite This Article 35 clicks
Cite This Article 35 clicks













Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.